The article below results from an interview with one individual, and is not intended as medical advice. Before embarking on any change to diet and exercise, first consult your doctor for advice.
Receiving a high blood pressure diagnosis when you’re in your late 50s is worrying in itself. Being told, at the same appointment, that you’re also pre-diabetic is a doubly wammy. Couple this bad news with the fact that you’re already slim, fit and eating what most people would consider to be a healthy diet, and you may find yourself thinking there’s no escape from a future of poor health and daily medication.
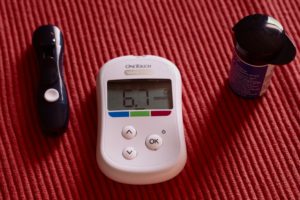 This was the case of Chris Philip (not his real name) when he visited his doctor for a regular check up. Already a vegetarian for many years, and with high blood pressure and type 2 diabetes in his genes, Chris at first didn’t know what he could do to help himself. But blood pressure medication was the last thing he wanted prescribed because he knew it was a treadmill he was unlikely ever to get off, and that prescription drugs can have serious side effects for some people.
This was the case of Chris Philip (not his real name) when he visited his doctor for a regular check up. Already a vegetarian for many years, and with high blood pressure and type 2 diabetes in his genes, Chris at first didn’t know what he could do to help himself. But blood pressure medication was the last thing he wanted prescribed because he knew it was a treadmill he was unlikely ever to get off, and that prescription drugs can have serious side effects for some people.
With these thoughts driving him, Chris threw himself into researching his condition, and read as much as he could about others in the same situation who had helped themselves. Although his salt intake was already very low, he reduced it even further by excluding added salt from his diet completely. It was ‘goodbye’ to the likes of Marmite, commercial sauces, takeaways and baking powder (which is high in sodium), and ‘hello’ to balsamic vinegar brewers yeast, salt-free mushroom stock and sodium-free raising agents. When he was away from home, he always took his own food with him, and was highly selective when it came to eating out.
Realising he was battling an extreme situation (given his already healthy lifestyle) Chris decided to follow a school of thought which said that a sufficiently high level of potassium can help mitigate the effects of even low levels of salt in a diet. As a vegetarian, Chris wasn’t short of potassium but he increased his intake even further by eating fresh, leafy greens at every meal – and in great quantities. Salads became his bulk – and he skipped the sweet and salty dressings.
Chris also began eating bitter greens such as chicory, and wild puha and dandelion. It is thought that bitter greens contain phytochemicals in high concentrations, and that these chemicals assist the flexibility of the arteries. ‘Bitter’ is a flavour that is enjoyed in many European countries, and although it is usually alien to the Kiwi diet, Chris eased himself into it by incorporating these special greens into his salads. Now, he enjoys them on their own.
Chris also took on board the suggestion that black and green tea, cocoa, nuts (including peanuts), berries, and beetroot help with artery flexibility.
After reading further, Chris decided to skip all extracted oils, olive oil included, because they are implicated in heart disease and because they are not ‘whole foods’ (there is evidence that the fibre in whole foods helps to even out blood sugar levels). Instead, he decided to get his oils (which are essential in the diet) from nuts and seeds. With the aim of controlling sugar intake, Chris limited his alcohol intake to less than a standard glass every two weeks, and went without refined sugar and honey.
Already a regular runner, Chris made the decision to continue with his sport and to make sure his fitness didn’t wane (although he says that any exercise which raises the heart rate and keeps it up for more than 10 minutes at a time is likely to be helpful).
Although the changes Chris made may seem extreme to many, his blood pressure has reduced to the lower end of normal, and he has staved off type 2 diabetes for over 7 years – and for that reason, he doesn’t plan to alter his lifestyle any time soon!








Join the Discussion
Type out your comment here:
You must be logged in to post a comment.